Division of Energy Employees Occupational Illness Compensation (DEEOIC)
This page contains resources to assist you with various components of the program. Below you will find links that provide program benefits and eligibility information, instructions on how to file a claim, and access to your claim status. The Energy Document Portal link provides guidance on how to submit documentation in support of your claim. In the Medical Bill Portal section, you will find medical forms along with instructions on how to complete the forms. The File a Home Health Care Claim link gives you the ability to retrieve Form EE-17A, which allows you to request home health care. The Impairment and Wage Loss links provide pertinent information regarding filing claims specific to those topics. Finally, the Forms link will direct you to the most commonly used forms in the program.
The Energy Employees Occupational Illness Compensation Program provides benefits authorized by the Energy Employees Occupational Illness Compensation Program Act (EEOICPA). Part B of the Program went into effect on July 31, 2001, and Part E of the Program went into effect on October 28, 2004. The Department of Labor's Office of Workers' Compensation Programs is responsible for adjudicating and administering claims filed by employees or former employees or certain qualified survivors.
Part B Eligibility
- Employees of the Department of Energy (DOE), its contractors or subcontractors who worked at a covered DOE facility during a covered time period
- Employees of atomic weapons employers
- Employees of beryllium vendors
- Uranium workers previously awarded benefits by the Department of Justice under Section 5 of the Radiation Exposure Compensation Act (RECA) for the same covered illness
Conditions Eligible for Compensation
- Radiogenic cancer
- Chronic Beryllium Disease
- Beryllium Sensitivity
- chronic silicosis
Under Part B, compensation includes a lump sum amount of $150,000 and payment of medical expenses from the date a claim is filed. If the employee is no longer living, the lump sum is payable to eligible survivors. Compensation is payable to eligible survivors in the following order: spouse, children, parents, grandchildren, and grandparents of the deceased covered employee.
Compensation of $50,000 and payment of medical expenses from the date a claim is filed is available for uranium workers (or their survivors) previously awarded benefits by the Department of Justice under Section 5 of the Radiation Exposure Compensation Act.
Employees of the Department of Energy, its contractors and subcontractors who were exposed to beryllium on the job and now have beryllium sensitivity will receive medical monitoring to check for Chronic Beryllium Disease.
Part B Lump-Sum Compensation Journey Map – The journey map is a visualization of the 'typical' stages that a claimant undergoes while their Part B claim is adjudicated.
Part E Eligibility
- Employees (or their survivors) who worked for a DOE contractor or subcontractor during a covered time period at a covered DOE facility
- Uranium miners, millers, and ore transporters as defined by RECA Section 5, or their survivors.
Eligible survivors include:
- A spouse who was married to the employee for at least one year prior to his/her death. If there is no surviving spouse, then compensation may be awarded to a covered child if, at the time of the employee's death, the child was:
- Under the age of 18
- Under the age of 23 years and a full-time student continuously enrolled in an educational institution, or
- incapable of self-support
Conditions Eligible for Compensation
Under Part E, benefits are provided for any illness if it can be determined that it was “at least as likely as not” that occupational exposure to a toxic substance was a significant factor in causing, contributing to, or aggravating the illness or death of an employee. Compensation under Part E is awarded for Wage Loss, Impairment and medical benefits.
Under Part E variable compensation up to $250,000 is determined based on wage loss, impairment, and survivorship.
Part E Impairment and/or Wage Loss Journey Map – The journey map is a visualization of the 'typical' stages that a claimant undergoes when filing for impairment or wage loss under Part E.
The Office of Workers’ Compensation Programs (OWCP) on behalf of the Division of Energy Employees Occupational Illness Compensation (DEEOIC) have combined everything that you will need in one location to navigate through the claims process. This section provides information through a step-by-step guide to file an employee or survivor claim for benefits. The section informs you of additional documentation needed from the start of the claims process to a final decision. The section also contains instructions on submitting forms and documentation to the DEEOIC. To file a claim, click one of the links below.
Employee
Are you filing a claim as a current or former covered employee under the EEOICPA?
Step-by-step guide to filing a Claim for Employee Benefits
The steps outlined here are intended as a "quick-start" guide for workers and former workers.
Step 1: Complete the application form titled, "Employee Claim for Benefits under the EEOICPA" (form EE-1).
Step 2: Complete the form titled, "Employment History" (form EE-3).
Step 3: Include any copies of supporting medical and employment documentation along with your application. DO NOT SUBMIT ORIGINAL DOCUMENTS.
Step 4: You have a few options to submit your claim Form.
- Access the Energy Document Portal (EDP) by visiting the EDP website at: https://eclaimant.dol.gov. Claimants can select a claim application form to complete, digitally sign, and submit to DEEOIC. Claimants using EDP to submit an EE-1 form must use this option to provide a valid digital signature; we are unable to accept scanned copies of these forms in EDP.
- Utilize Resource Center assistance. There are 11 Resource Centers located across the country. Assistance can be provided at any office, regardless of location. The Resource Centers provide assistance either in person or over the phone.
By mail to:
U.S. Department of Labor OWCP/DEEOIC
P.O. Box 8306
London, KY 40742-8306
Survivor
Are you filing a claim as the survivor of a covered employee under the EEOICPA?
The steps outlined here are intended as a "quick-start" guide for the survivors of workers and former workers.
Step 1: Complete the application form titled, "Survivor Claim for Benefits under the EEOICPA" (form EE-2).
Step 2: Complete the form titled, "Employment History" (form EE-3).
Step 3: Include any copies of supporting medical, employment, and survivor documentation along with your application. DO NOT SUBMIT ORIGINAL DOCUMENTS.
Step 4: You have a few options to submit your claim Form.
- Access the Energy Document Portal (EDP) by visiting the EDP website at: https://eclaimant.dol.gov. Claimants can select a claim application form to complete, digitally sign, and submit to DEEOIC. Claimants using EDP to submit an EE-2 form must use this option to provide a valid digital signature; we are unable to accept scanned copies of these forms in EDP.
- Utilize Resource Center assistance. There are 11 Resource Centers located across the country. Assistance can be provided at any office, regardless of location. The Resource Centers provide assistance either in person or over the phone.
By mail to:
U.S. Department of Labor OWCP/DEEOIC
P.O. Box 8306
London, KY 40742-8306
Things You Need to Know:
What Happens after I File a Claim?
What Compensation is Available under the EEOICPA?
Can I Have Someone Represent Me?
What Happens after I receive a Recommended Decision?
I Just Received a Final Decision. What Do I do Next?
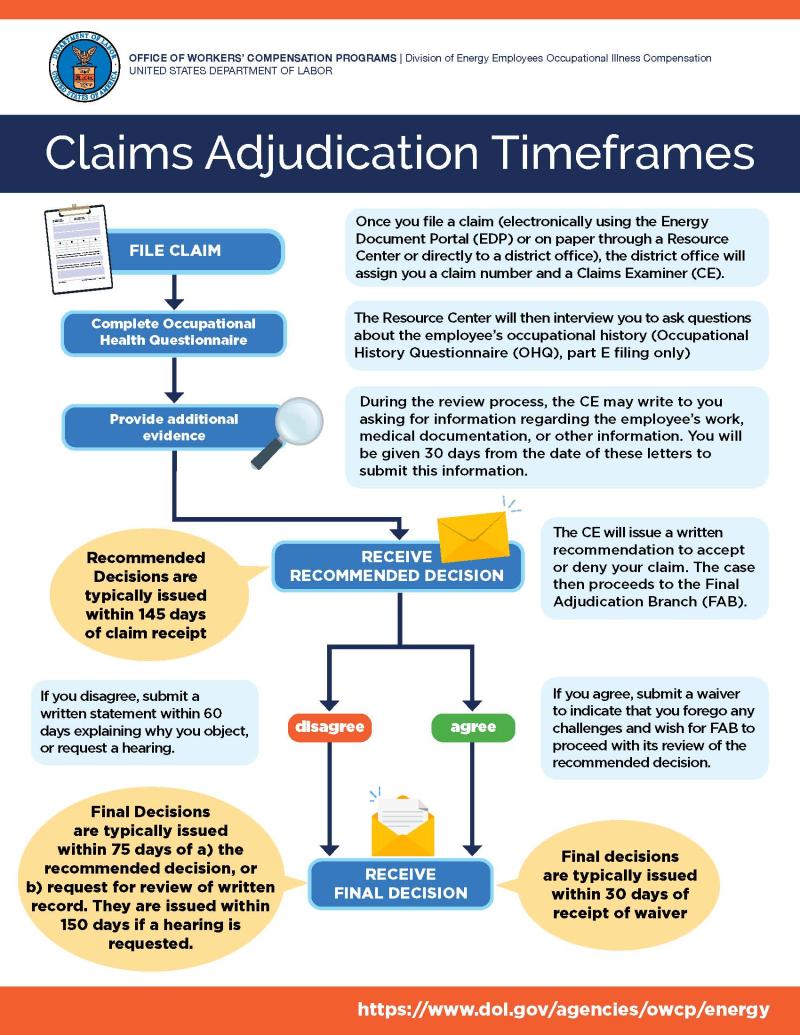
What Happens after I File a Claim?
DEEOIC will issue you a claim number and it will create an official file to assemble case records. It will also assign a Claims Examiner (CE) to your claim. The CE is responsible for managing your claim during the decision-making process. The CE role requires that they review evidence to determine if your claim satisfies the legal requirements for awarding compensation benefits. In situations when the CE needs to obtain more documentation to support a claim, he or she will mail you requests for needed evidence or information. Upon collection of all available evidence, the CE will issue a written recommendation to either accept or deny your claim. The Final Adjudication Branch (FAB) will then review the recommendation to decide whether it can finalize the acceptance or denial of your claim.
What Compensation is Available under the EEOICPA?
Under Part B, the maximum lump sum compensation is $150,000 plus medical benefits. RECA Section 5 recipients who received $100,000 from the Department of Justice may be eligible for $50,000, plus medical benefits. Under Part E, an employee maybe eligible for wage loss and/or impairment with a maximum compensation of $250,000, plus medical benefits. For survivors the maximum benefit amount is $125,000. A survivor may be entitled up to an additional $25,000 or $50,000 depending upon the amount of calendar years over 10 years that the deceased covered employee experienced compensable wage-loss prior to his or her normal Social Security retirement age.
Can I Have Someone Represent Me?
Yes, you may elect to have someone represent you. Many claimants choose to have a trusted family member or other close associate serve as a representative. Others decide to pay someone with professional or legal experience to be their representative. It is not necessary for you to name a representative; however, if you do decide to name a representative, it is important to select a person who will serve your best interest. You may select one person to serve as a representative. The selection of your representative must be in writing and list the authorized representative’s (AR’s) full name, telephone number, and address. Once DEEOIC receives your written selection of a representative, the representative will have the authority to submit and receive documents on your behalf, communicate with program staff, and make decisions regarding how best pursue your claim. DEEOIC permits one representative to serve at any one time, but you may change representatives at any time, so long as the request is in writing. For more information regarding representative services, view our brochure:
Using the Services of an Authorized Representative
What professional conduct expectations should I have related to the actions of my chosen Authorized Representative?
The Office of Workers’ Compensation Programs (OWCP) has published in the Federal Register, the OWCP Expectations of Conduct, which apply to all Authorized Representatives and how they are expected to interact on your behalf with our staff. Those standards are available here.
What Happens after I receive a Recommended Decision?
It is important to always first carefully read and understand any decision issued by the DEEOIC to you. The recommended decision communicates the reason(s) why the program is accepting or denying a claim. It may include action on all or some of the parts of your claim. The recommended decision will also include written instructions about your responsibilities depending on whether you agree or disagree with the decision. In any situation where you or your representative do not understand a recommended decision or the actions you need to take in response to a recommended decision, immediately contact the district office responsible for your claim.
Once DEEOIC issues a recommended decision, it will mail the decision to you and your authorized representative. DEEOIC will also add a copy of the decision to your permanent case record. The Final Adjudication Branch (FAB) then takes possession of your case to await any new information submitted in response to the recommended decision. FAB is a separate and independent organization within DEEOIC whose responsibility is to decide whether to finalize the recommendation decision. Once FAB assumes responsibility of your claim, you will need to decide whether you agree or disagree with the recommended decision. FAB allows for up to 60 days for you to notify it that you have no objection to the recommendation or that you wish to contest the recommendation. If you do not have any objection, you will need to submit a document called a waiver that tells FAB that you are forgoing any challenge to the recommendation and indicating to FAB that you want it to proceed with its review of the recommendation. In those situations where you disagree with the recommendation, you have a choice to submit a written statement explaining why you object to the recommendation or you may ask for the chance to explain your objection at an oral hearing. In pursuing any objection to a recommendation, you will have the opportunity to submit any new evidence you wish FAB to consider before it renders its decision. At the conclusion of FAB’s review process, regardless of whether you object to the recommendation or not, it will conduct a comprehensive review of all the evidence of file to decide if the recommendation decision complies with the legal requirements of the EEOICPA. Either FAB will then issue a final decision that finalizes the recommendation or it issue a decision called a remand. A remand is a decision that communicates FAB’s disagreement with the recommended decision due to the receipt of new evidence or other identified deficiencies. Once FAB issues a remand, it will return your case file to the office that issued the recommended decision for more development.
I Just Received a Final Decision. What do I do Next?
Read the decision carefully. The final decision explains the evidence FAB considered in finalizing a recommendation to accept or deny your claim. It also provides instruction on the steps you need to take based on the decision outcome. Awards of monetary compensation require the submission of specific documents to allow for payment to your bank account. Information regarding medical benefits will include guidance on the conditions DEEOIC has accepted for workers’ compensation coverage and how you obtain reimbursement for medical care of an accepted condition. The final decision will also include specific instruction for appealing decisions for which you disagree. If you disagree with your Final Decision, you have the right to request reconsideration or file a request to reopen your claim. A request for reconsideration must be received 30 calendar days after the date of issuance of the Final Decision. A request for reopening may be submitted at any time after the issuance of a Final Decision.
The Claimant Status Page allows claimants to access certain information contained in his or her claim under the Energy Employees Occupational Illness Compensation Program (EEOICP). The Claimant Status Page makes information available online to claimants regarding their claimed medical conditions, worksite locations, most recent claim action, payment information, and current case location. Claimants under the EEOICP will be provided with an individual claim identification number to gain access to their claim information and to prevent the access by other individuals to a claimant’s specific claim information. In order to log in, the claimant will be asked to provide the last four digits of the Employee’s social security number/Case number; your date of birth; and your unique Claim Identification number. Once you have your unique Claim Identification number, if you have questions or concerns, you can contact the District Office handling your claim.
The Energy Document Portal (EDP) is an electronic document submission system that allows Energy Employees Occupational Illness Compensation Program Act (EEOICPA) claimants to file a new or consequential claim, complete wage loss or impairment forms, file benefit payment forms, electronically submit documents to their existing case file, and/or verify that documents were successfully submitted. Documents submitted within EDP are available to DEEOIC claims staff immediately after the document upload is complete, thus eliminating the mailing delays.
Use of the EDP is voluntary. If claimants do not wish to electronically upload documents into the EDP, they may continue to mail documents to the Central Mail Room (CMR) or bring their documents to the nearest DEEOIC Resource Center where they will be uploaded into OIS. Claimants should include the DEEOIC Case ID number on all documents mailed to the CMR. The address for the CMR is:
U.S. Department of Labor OWCP/DEEOIC
P.O. Box 8306
London, KY 40742-8306
Click on the link below to access a brochure that contains additional information regarding the EDP. You may also access the EDP login page by clicking the link below.
The Medical Bill Portal for Office of Worker’s Compensation Programs provides information regarding the DEEOIC EEOICPA. In the portal you have access to medical forms and instructions. You can find instructions that detail how to submit travel refund request, dental claim forms, pharmacy claims forms and other medical claim forms in order to receive timely reimbursements. The portal as well as other information about medical benefits can be accessed by clicking the links below.
For claimants that have been approved under the EEOICPA and awarded medical benefits for a work-related conditions(s), and wish to request home health care, assisted living, or nursing home benefits, you must complete form EE-17A. You can find answers to frequently asked questions and more information by clicking here: Home and Residential Health Care Services Brochure.
**Please Note: The EE-17A form is required for new requests only and not required if you are seeking reauthorization of benefits**
Step 1: Complete the EE-17A form in its entirety, titled, “Claim for Home Health Care, Nursing Home, or Assisted Living Benefits under the Energy Employees Occupational Illness Compensation Program Act.”
Step 2: Use Blue or Black Ink only. Write clearly and within the boxes provided. Please complete all sections of the form. Missing or incomplete information may result in processing delays.
Step 3: Employee’s Information: Either the covered employee, authorized representative or power of attorney must complete this section.
Step 4: Type of Medical Benefit: Select the type of care you would like to request.
Step 5: Treating Physician: Provide your treating physician’s name and contact information. This is the physician responsible for providing care related to the accepted work-related condition(s). Please note that the physician must be either an M.D. or D.O.
Step 6: The quickest way to have the form added to your case is to upload it to the Energy Document Portal. You can also submit claim forms through the Resource Centers or the District Offices, via U.S. mail. There are total of 11 Resource Centers located across the country that are equipped to assist claimants either in person or over the phone.
“Ancillary Medical Benefits Journey Map – The journey map is a visualization of the 'typical' stages that a claimant undergoes when filing for Ancillary Medical Benefits. Ancillary Medical Benefits include Home and Residential Health Care, Durable Medical Equipment, Rehab, Home/Vehicle Modifications, and Medical travel over 200 miles.”
An impairment award is monetary compensation available under Part E of the EEOICPA for the permanent loss of function of a body part or organ, due to a covered illness under the EEOICPA, as established by medical evidence and measured by percentage points. This section informs you of your eligibility for benefits and how to file for impairment. You may complete and submit the impairment form as a hard copy or use the Energy Document Portal (EDP) to complete and submit your form electronically. Click on the links below for a brochure on impairment and forms to request impairment.
How Do I Qualify for an Impairment Award under Part E of the EEOICPA?
EN-11A Impairment Benefits Response Form
EN-10 Claim for Additional Wage-Loss and/or Impairment Benefits Under the EEOICPA
Under the EEOICPA, wage-loss compensation is payable under Part E of the EEOICPA for those years the employee experienced loss of wages before his or her Social Security Administration (SSA) regular retirement age. You may complete and submit the wage loss form as a hard copy or use the Energy Document Portal (EDP) to complete and submit your form electronically. The link below has a brochure that discusses eligibility and how to file for wage loss benefits. Additionally, you will find an example wage loss compensation forms below.
How do I qualify for Wage Loss Benefits under Part E of the EEOICPA
EN-11B Wage-Loss Benefits Response Form
EN-10 Claim for Additional Wage-Loss and/or Impairment Benefits under the EEOICPA
The Director of the Division of Energy Employees Occupational Illness Compensation (DEEOIC) has the authority to reopen a claim and vacate a Final Decision at any time after its issuance by the Final Adjudication Branch (FAB). A claimant that is party to the decision may request that the Director consider a reopening of a Final Decision if the claimant disagrees with its outcome. In certain circumstances, the Director may delegate the authority to address a reopening request to the Policy Branch Chief or a District Director of one of the DEEOIC District Offices.
A claimant may request a reopening for any reason. However, there must be sufficient justification provided by a claimant to warrant vacating a Final Decision including the presentation of new information or evidence. In most instances, a reopening request that is unaccompanied by any new evidence or argument will not result in change to a Final Decision.
Below are some examples of reasons the DEEOIC may reopen a claim. This is not an all-inclusive list. Other reasons for reopening a claim are possible.
- Evidence of additional periods of covered employment.
- Newly obtained diagnostic or clinical evidence establishing a diagnosis for a condition previously denied due to insufficient medical evidence.
- Addition of newly diagnosed primary cancer(s) that may affect the Probability of Causation (PoC) for a claim that DEEOIC referred to the National Institute for Occupational Safety and Health (NIOSH) for a radiation dose reconstruction.
- Documentation clarifying a survivor’s relationship to the employee
- New data relating to toxic substances encountered by the employee at work that resulted in a claimed illness(es) including updates to information reported in DEEOIC’s Site Exposure Matrix (SEM).
- Presentation of a new medical opinion that links a claimed illness to an occupational toxic substance exposure
- Change in Law, Regulations, or Policies.
Once DEEOIC receives a reopening request, the Director or a delegated authority will review the request, along with any new evidence or argument, and issue a Director’s Order to reopen the claim or issue a Denial of Reopening Request. The typical timeframe to receive a decision on a reopening request is 90 days or less from the date DEEOIC receives it.
Step-by-step guide to Requesting a Reopening
Step 1: Prepare and sign a written request communicating clearly your intent to seek a reopening of a prior final decision. Be as specific as possible with the request including the identification of the final decision under contention. Describe the reasons for contesting the final decision and explain how any new evidence or argument justifies a reopening.
Step 2: Collect and make a copy of any additional evidence supporting the requested reopening, such as new medical, employment and survivor documentation.
Step 3: Submit your written request for reopening and any additional evidence for consideration to DEEOIC. It is unnecessary to submit original versions any documents to DEEOIC. DEEOIC accepts document copies.
You have several options to submit your reopening request. You can submit your request by mail, through the Energy Document Portal or by contacting the Resource Center for assistance. There are 11 Resource Centers located across the country. The Resource Centers can provide assistance at any office, regardless of location, either in person or over the phone.
This section has access to the most commonly used forms under the EEOICPA. The forms may be completed and submitted by mail, through one of the 11 Resource Centers or through the Energy Document Portal. Forms submitted through the EDP can only be uploaded after you have been assigned a claim number. After a claim number has been issued, Forms EE-3, EE-4 and EE-7 can be uploaded into EDP. Please do not submit EE-1 or EE-2 claim forms via EDP. New claims should be submitted to the Resource Center or to the Central mail Room.
U.S. Department of Labor OWCP/DEEOIC
P.O. Box 8306
London, KY 40742-8306
Click on any of the links below to access frequently used forms.
- Employee's Claim: Form EE-1
- Survivor's Claim: Form EE-2
- Employment History: Form EE-3
- Employment History Affidavit: Form EE-4
- Physician/Provider Billing Form: OWCP-1500
- Reimbursement for out-of-pocket medical expenses: OWCP-915
- Uniform Billing Form for Medical Services: OWCP-04
- Medical Travel Refund Request – Mileage: OWCP-957 Part A
- Medical Travel Refund Request – Expenses: OWCP-957 Part B
- Direct Deposit Sign-up Form SF-1199A
- Claim for Home Health Care, Nursing Home, or Assisted Living Benefits: Form EE-17A
- Physician’s Certification of Medical Necessity: Form EE-17B