OCA's third aspect consists of the OCA enforcement programs to ensure compliance with ERISA's reporting and disclosure requirements.
The Office of the Chief Accountant (OCA) is delegated the responsibility of ensuring that plan administrators completely and accurately comply with the reporting requirements under Title I of ERISA. Failure to file a timely and accurate Form 5500 can be indicative of poor plan management and at-risk participants.
ERISA §104(a)(4) permits the Secretary of Labor to reject any filing that she determines to be incomplete or deficient.
OCA has a number of established enforcement programs to ensure compliance. There are two goals for the OCA enforcement programs. The first goal is to improve the overall quality of the independent audits of employee benefit plans required by ERISA in order to facilitate the protection of plan assets and the related benefits of plan participants and beneficiaries. The second goal is to ensure that plans are in compliance with the reporting and disclosure requirements of ERISA, and that deficient Forms 5500 filings are corrected. Accordingly, OCA strives not only to improve the independent audit process but also to improve the accuracy of plan reporting and disclosure.
OCA's enforcement programs include:
- Audit Quality Inspection Programs
- Augmented Workpaper Review
- On-site Workpaper Review
- Deficient Filer Enforcement
- Non-Filer Enforcement Program
- Late Filer Enforcement Program
- Delinquent Filer Voluntary Compliance Program
OCA's other Delegated Enforcement Programs include:
- Multiple Employer Welfare Arrangements Program
- Section 502(c)(6) Document Compliance Program
- Blackout Notice Provision Program – Section 502(c)(7)
- Section 502(c)(8) – Failure to establish a funding improvement plan
- Section 502(c)(4) – Failure to furnish a withdrawal liability notice
Audit Quality Inspection Programs
One of OCA's greatest challenges is the fact that more than 10,000 CPA firms audit the nation's retirement and health plans.
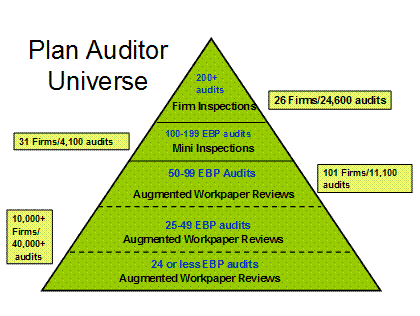
The Audit Quality Inspection Program represents an expanded inspection of the IQPA over DAS' former traditional on-site audit workpaper reviews. The program consists of two main parts: 1) top-down review of IQPAs' Employee Benefit Plan Audit Practices; and 2) review of a sample of the IQPAs' employee benefit plan audit workpaper engagements.
Due to its limited resources, DAS looks more closely at the IQPAs performing a significant number of benefit plan audits and/or audit the majority of the plan asset population. If there is a problem with one of the IQPAs in this group, a greater percentage of plan assets and plan participants could be affected as compared with IQPAs that are less active in the employee benefit plan sector. Firms that conduct more than 100 employee benefit plan audit engagements or IQPAs that audit a significant amount of plan assets are subject to DAS' Audit Quality Inspection Program.
For IQPAs selected for review as a part of this program, DAS performs an inspection of the IQPA's employee benefit plan audit practices. This inspection includes, among other things, reviewing and documenting whether or not the firm has designated an audit partner who has firm-wide responsibility for the quality of the firm's ERISA employee benefit plan audit practice; whether the firm has an established program to ensure that all personnel assigned to the ERISA employee benefit plan audit engagement personnel possess technical knowledge appropriate to the level of involvement in the audit engagement; whether the firm has established policies and procedures to ensure compliance with established professional standards; and whether the firm has an internal inspection program that includes a review of its employee benefit plan audit engagements to ensure audit quality and compliance with professional standards and ERISA and Department of Labor rules and regulations for reporting and disclosure for employee benefit plans. These inspections are typically conducted at the firm's national/corporate headquarters.
During the inspection process, DAS obtains a list of all of the firm's employee benefit plan audit clients. From this list, DAS then selects a random number of audit engagements for review of the audit workpapers to assess audit quality and compliance with professional standards and regulatory requirements. The engagements selected for review encompass a range of plan types (defined contribution, defined benefit, health & welfare, ESOPs), audit scope (limited scope & full scope audits) and plan investment risk factors (hard to value assets such as real estate and limited partnerships, non-marketable securities, etc.). If the IQPA maintains multiple offices, DAS selects its sample of plans for review from a number of office locations.
DAS carries out this program two ways, depending upon the number of employee benefit plan audit engagements performed by an IQPA firm.
- Firm-Inspection: For those firms that audit greater than 200 plans, DAS visits the headquarters of the firm and conducts the top-down component of the inspection. In addition, the review of the selected engagements is performed on-site at the firm's offices selected for review.
- Mini Inspections: For those firms that audit between 100 and 200 employee benefit plans, while subject to the same inspection, all parts of the review will be conducted in-house within the DAS office.
The audit engagements selected for review will be the most current audit engagement performed for the employee benefit plan selected.
Augmented Workpaper Review Program
Based on certain targeting criteria, DAS selects a number of employee benefit plan audits for an augmented workpaper review. DAS periodically reviews and reconsiders its methods of targeting plan audits in order to most efficiently accomplish its goals with the resources it has been provided. Generally, however, plans selected for review as a part of the augmented workpaper review program are plan(s) that have been audited by a firm that conducts less than 100 plan audits annually.
Augmented workpaper reviews of Form 5500s include the review of the Form 5500, a review of the related auditor's report for compliance with GAAS, GAAP and the regulatory reporting and disclosure requirements and a review of the underlying audit workpaper documentation prepared by the plan's IQPA in support of the audit opinion rendered. The workpaper documentation selected for review is determined on a case-by-case basis and may be limited to selected audit areas or all audit areas.
Where a plan has been selected for an augmented workpaper review, a review of the Form 5500 and related auditor's report is performed to determine compliance with GAAS, GAAP and the regulatory reporting and disclosure requirements. The analyst will review the audit report and will make a determination as to which relevant audit areas should be selected for a review. The audit areas selected for review will generally include those areas of audit where it has been historically demonstrated that errors are most likely to exist. These areas of audit include:
- assessment of the risk of fraud,
- investments & investment transactions,
- contributions received & receivable,
- benefit payments,
- participant data,
- plan obligations, and
- party-in-interest/prohibited transactions.
However, workpapers in other audit areas may also be requested if the analyst determines that the augmented workpaper review should include areas of audit in addition to those above. For example, the analyst may determine after a review of the Form 5500 and audit report that conditions exist which call into question whether or not the auditor has conducted a quality audit of the employee benefit plan. In such cases, the analyst may request copies of all of the audit workpapers or may request workpapers in areas in addition to those above.
After the analyst has determined which relevant audit areas will be reviewed, the analyst notifies the plan administrator that the respective plan has been selected for an augmented workpaper review. The DAS analyst will then request that copies of the audit workpapers associated with the relevant audit areas selected for review be provided to DAS.
Audit engagement(s) selected for an augmented workpaper review will be the most current audit engagement(s) performed for the employee benefit plan selected. Augmented workpaper reviews are conducted within DAS' office.
On-Site Workpaper Review Program
Based on certain targeting criteria and/or a review of the Form 5500 and related audit report, DAS may periodically select an employee benefit plan audit for an on-site review of the IQPA's workpapers. DAS periodically reviews and reconsiders its methods of targeting plans in order to most efficiently accomplish its goals with the resources it has been provided.
Where a plan has been selected for an on-site workpaper review, a review of the Form 5500 and related auditor's report is performed to determine compliance with GAAS, GAAP and the regulatory reporting and disclosure requirements. In addition, the analyst notifies the plan administrator that the respective plan has been selected for an on-site review and a request is made for access to the IQPA's workpapers that were prepared in support of the audit opinion rendered on the plan's financial statements. The DAS analyst then schedules a date and time to review the IQPA's workpapers. The on-site review is typically conducted at the IQPA's office.
Audit engagement(s) selected for an on-site workpaper review will be the most current audit engagement performed for the employee benefit plan selected.
Deficient Filer Enforcement Program
The Deficient Filer Enforcement Program is historically OCA's primary program. The program is conducted primarily through correspondence detailed in 29 CFR §2560.502c-2.
The Form 5500 is a valuable tool used by many organizations to monitor the safety of plans and identify current plan trends. The information is also important to the plan's participants. Without this information, it is difficult to assess the stability of a plan. In order to ensure a plan is being maintained in a responsible manner, the Form 5500 is used to get a reporting of the plan's activities over the previous year.
OCA's primary objective in the deficient filer compliance program is to ensure the information reported on the Form 5500 is complete and compliant with the annual reporting regulatory requirements. This information is stored within the EFAST database, which is then utilized by EBSA, other agencies of the Department of Labor, other Departments and outside groups for the purpose of oversight and monitoring, research, and compilation of statistical data.
Based on certain targeting criteria, OCA selects a number of Form 5500s for desk review. OCA periodically reviews and reconsiders its methods of targeting plan audits in order to most efficiently accomplish its goals with the resources it has been provided. Plans selected for review as part of the Form 5500 desk review enforcement program involve a review of the Form 5500 and/or related auditor's report for compliance with GAAS, GAAP and ERISA and Department of Labor reporting and disclosure requirements. Typical deficiencies that are targeted include missing/deficient audit reports and Schedule of Assets Held. With the advent of the EFAST database, targeting by OCA has become far more detailed and timely. As of 2006, OCA also began targeting on significant changes assets, failure to secure the proper bonding, and hard to value assets.
Cases initiated by DRC consist of a detailed review of the entire filing. Cases initiated by DAS consist mainly of a detailed review of the audit report for compliance with professional standards and reporting and disclosure requirements.
Direct Filing Entity Enforcement Program
Some plans invest in certain trusts, accounts and other investment arrangements that may file information concerning themselves and their relationship with employee benefit plans directly with the DOL. These entities are referred to as "direct filing entities" (DFEs) and include master trust investment accounts (MTIAs), common or collective trusts (CCTs), pooled separate accounts (PSAs), 103-12 investment entities (103-12 IEs) and group insurance arrangements (GIAs). MTIAs and 103-12 IEs must file directly with the DOL for participating plans' filings to be deemed complete. Although GIAs, CCTs and PSAs are not required to file directly with the DOL, their decision not to file affects the filing requirements and manner in which information is reported by participating plans on their Form 5500s.
DFEs are required to submit their information using the Form 5500 Annual Report. The EFAST system processes and summarizes the data contained in these filings in a standardized manner. With access to this data, OCA has created and implemented a program to ensure that DFEs, and plans that participate in them, meet their reporting and disclosure obligations.
An integral part of EBSA's mission is to "take regulatory and enforcement actions that will be protective of the interests of the participants and beneficiaries and will encourage the creation and maintenance of plans." OCA's DFE Enforcement Program seeks to protect the interests of participants and beneficiaries by:
- scrutinizing DFE Form 5500 Annual Reports to deter and correct violations of relevant statutes;
- ensuring that DFE Form 5500 Annual Reports are filed timely and accurately; and
- ensuring that, where required, audits of DFE entities comply with established professional standards.
Under the DFE Enforcement Program, Form 5500 Annual Reports are reviewed from two different perspectives: (1) Beginning with the DFE Form 5500 Annual Report and ending with the individual Form 5500 Annual Report filings for participating plans and (2) Beginning with the individual Form 5500 Annual Report filings for participating plans and ending with the DFE Form 5500 Annual Report.
For example, a Form 5500 Annual Report is filed for a MTIA. The analyst reviews this filing to ensure that it is timely, accurate and complete. Form 5500s filed for MTIAs must include the employer identification number and plan number of each plan participating in the MTIA on Schedule D, Part II. As a result, OCA is able to compare the MTIA filing to the individual plan filings listed on Schedule D, Part II, to ensure that all the information has been properly reported and disclosed on both the MTIA Form 5500 and the Form 5500s for the individual plans participating in the MTIA.
The reverse analysis can also be performed. For, example, a plan indicates in its Form 5500 filing that it has investments held in a MTIA. Plans with investments in DFEs must include the employer identification number and plan number of each DFE on Schedule D, Part I. As a result, OCA is able to compare the plan filing to the DFE filing listed on Schedule D, Part I, to ensure that all of the information has been properly reported and disclosed on both the plan's filing and the associated DFE filing(s).
Since the Form 5500 filed for a DFE is an integral part of the Form 5500 for each plan participating in the DFE, deficiencies identified in a DFE filing may cause the associated plan filings to be deficient and, therefore, subject to rejection by the DOL. It should be noted that while the DOL cannot "reject" a DFE filing, DFEs reviewed as a part of this program are notified that their deficient DFE filing may result in rejection and possible civil penalties assessed on all of the participating plans' Form 5500 filings unless an acceptable filing is made for the DFE. If the DFE fails to provide a satisfactory Form 5500 filing for the DFE, OCA may proceed with an enforcement action against the plan administrator of the associated plans.
Non-Filer Enforcement Program
One of the primary missions of OCA is to ensure proper reporting and disclosure of plan activities through the Form 5500 annual reporting process. EBSA has long believed that the failure to file an annual report is one the most egregious violations of ERISA. Therefore, one of the OCA's enforcement efforts is to identify plans that have a filing requirement but have not filed and bring them into compliance with ERISA. A plan that is required to file an annual report but has never filed a report is called a "non-filer". A plan is considered to be a "stop-filer" when it has filed in the past but has since stopped filing annual reports.
Without the information on the Form 5500, it is difficult to determine the health of a plan. For this reason, timely filing is of the utmost importance. It is the goal of OCA to achieve timely and accurate filings for all plans. Non-filers, being at the most risk of abuse, receive the highest penalties.
There are various methods used to identify non-filers and stop-filers. Historically, the majority of non-filers were referrals from either the Office of Enforcement or the IRS. A few also came from other sources such as the Division of Technical Assistance & Information.
Stop-filers have been identified through referrals and queries of the EFAST database. The queries compare prior year filings to current year filings and identifies plans that filed in a prior year but did not file in the current year. Filings that indicated the plan was being merged or terminated are excluded from these queries.
Referrals from other offices are reviewed to determine the validity prior to opening and assigning a case to an analyst.
Late Filer Enforcement Program
DRC began the late filer program in the early 1990s after the 1992 Grace Period. During that program, it was discovered that a large number of plans were filing their Form 5500s past the due date which is 7 months after the end of the plan year. Much of the value of the information on the Form 5500 is its timeliness. The goal of the late filer program is to encourage future timely filing.
The penalty for late filers is $50 per day from the day the filing was due until the day filed without regard to extensions.
Delinquent Filer Voluntary Compliance Program
Introduced in 1995 and revised in 2002, the Delinquent Filer Voluntary Compliance (DFVC) Program is designed to encourage plan administrators to file previously unfiled Form 5500 Series annual reports and to resolve potential late filer penalties.
After a highly successful 1992 grace period program that collected over 40,000 filings during a nine month period, plan administrators who had missed the grace period were apprehensive about filing unfiled or late Form 5500s for fear of significant penalties that could be imposed. With this in mind the original DFVC penalty was structured above the Grace Period amount ($1,000 per filing) but well below potential late and non-filer penalties. The DFVC program is now an ongoing program with no anticipated end date.
The DFVC program was revised on March 28, 2002. The 2002 revision reduced the "per day" penalty rate and per filing penalties; the created a per plan cap and the created a special class of filers, and it aligned the DFVC filing procedures with the new EFAST system. The DFVC program has been modified recently for the EFAST2 procedures.
In order to participate in the DFVC program, a plan administrator must complete all of the following:
- File a complete electronic filing in EFAST2 (see, Frequently Asked Question Q4 EFAST2 All-Electronic Filing System)
- Top Hats and ATPs must mail a statement to the Department, not EFAST.
- Remit payment in accordance with the Department applicable requirement http://www.dol.gov/agencies/ebsa/about-ebsa/our-activities/resource-center/faqs/dfvcp. Send in a check for the penalty amount to the post office "lock box" address noted on the DFVC Website or pay the penalty amount electronically.
(Top Hat and ATP filers must complete 1a-c, 2a-c, 5a-c, and 6a or b on the 1998 or earlier Form 5500 and line items 1a-b, 2a-c, and 3a-c on the 1999 or later Form 5500. The plan number for Top Hats is 888 and for ATPs is 999.) If filing as a member of the special class, the plan must write "501(c)(3) organization" at the top of each filing.
The penalties under the DFVC program are:
| Per Filing | Per Plan | |
|---|---|---|
| Large Form 5500 Filers | $10/day up to $2000 | $4,000 |
| Small or Form 5500 C Filers | $10/day up to $750 | $1,500 |
| Top Hat Plans | $750 regardless of the number of plans | |
| Apprenticeship & Training Plans | $750 regardless of the number of plans | |
| Small 501(c)3 Plans | $10/day up to $750 | $750 |
If the Department of Labor has notified a plan of its intent to assess a penalty for the failure to file timely annual report then the plan is no longer eligible for the DFVC program. If the filer receives a notice from the IRS, the administrator remains eligible for the program; however, the IRS is not required to waive their penalties after they have issued a letter.
Incoming Mail and Information
The Department's lockbox agent is responsible for receiving the DFVC submissions and the depositing of the payments and data entry of the records. Once this is completed, the scanned images of the filings are transmitted to the Department of Treasury for viewing. At the same time, the computer record is posted on their Website which is then uploading by DRC everyday.
Multiple Employer Welfare Arrangements Program
According to §3(40) a Multiple Employer Welfare Arrangement ("MEWA") is an employee welfare benefit plan, or any other arrangement, that is established or maintained for the purpose of offering or providing welfare plan benefits to employees of two or more employers (including one or more self-employed individuals) or their beneficiaries. However, a MEWA may not be any plan or arrangement which is established or maintained:
- under or pursuant to one or more arrangements which the Secretary of Labor finds to be collective bargaining agreements;
- by a rural electric cooperative; or
- by a rural telephone cooperative association.
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) added a new §101(g){h} to ERISA, giving the Secretary of Labor authority to require reporting by MEWAs that are not group health plans. HIPAA also added a new section 502(c)(5) to ERISA, authorizing the Secretary to impose a civil monetary penalty against any person of up to $1,000 a day from the date of the person's failure to file a report required under section 101(g)(h) of ERISA.
On April 9, 2003 the final rules governing certain reporting requirements under Title I of ERISA for MEWAs and certain other entities that offer or provide coverage for medical care to the employees of two or more employers were published in the Federal Register.
- 29 CFR 2520.101-2 generally requires the administrator of a MEWA, and certain other entities, to file a Form M-1, Annual Report for Multiple Employer Welfare Arrangements and Certain Entities Claiming Exception, with the Secretary of Labor for the purpose of determining whether the requirements of certain recent health care laws are being met. The administrator of the MEWA or Entity Claiming Exception (ECE) is required to file the Form M-1 within 90 days of the date the MEWA or ECE is originated. Also, the administrator of the MEWA or ECE is required to file the M-1 for each calendar year during all or part of which the MEWA or ECE offers or provides coverage for medical care. The M-1 is due on March 1st that follows a period to be reported. There is a 60 day automatic extension which may be requested no later than the normal due date for the Form M-1.
- 29 CFR 2560.502c-5 implements the Secretary's authority to impose civil penalties under ERISA § 502(c)(5). The penalties may not exceed $1,100 per day and are assessed against the MEWA or ECE administrator.
- 29 CFR 2570 Subpart E establishes procedures for administrative law judge proceedings in connection with §502(c)(5) penalties.
Under §101(g), MEWAs that provide medical benefits are subject to annual reporting requirements (i.e., filing Form M-1, generally by March 1st). A MEWA may or may not be an ERISA-covered employee welfare benefit plan. Under the Department's regulations at §2520.101-2, all MEWAs must file Form M-1; however, the §502(c)(5) civil penalty is enforceable only with respect to non-plan MEWAs. "Plan-MEWAs" are subject to the § civil penalty, for failure to file Form 5500.
Whether a MEWA is an ERISA-covered plan depends on whether the MEWA meets the definition of an employee welfare benefit plan set forth in section 3(1) of ERISA. This definition establishes a two–step test. First, the MEWA most provide welfare benefits, such as medical benefits. Second, the MEWA must be established or maintained by an employer, employee organization or both. DRC refers cases to the Office of Regulations and Interpretations when a determination is needed regarding MEWAs that claim that they are ERISA-covered plans.
There are various sources from which cases are selected and assigned to the analysts. A majority of the non-filers are referrals from the Office of Enforcement. To locate possible non-filers and late filers, a query is run on the ERISA database.
Stop filers are identified through a report run by the Department's targeting system, comparing the most recent year's filing information against the year before that. The report is looking for anybody who filed the first year but not in the second and did not indicate they were terminating the arrangement.
Late filers are identified through a report run by the Department's targeting system, looking for filings that were filed at least 100 days after the original due date. (There is a 60 day automatic extension which may be requested no later than the normal due date for the Form M-1.)
502(c)(6) Compliance Program
ERISA §104(a)(6) states, "The administrator of any employee benefit plan subject to this part shall furnish to the Secretary, upon request, any documents relating to the employee benefit plan, including but not limited to, the latest summary plan description (including any summaries of plan changes not contained in the summary plan description), and the bargaining agreement, trust agreement, contract, or other instrument under which the plan is established or operated.".
Effective March 8, 2002, OCA was delegated the authority to assess civil penalties under ERISA §502(c)(6), which states, "If, within 30 days of a request by the Secretary to a plan administrator for documents under §104(a)(6), the plan administrator fails to furnish the material requested to the Secretary, the Secretary may assess a civil penalty against the plan administrator of up to $100 a day from the date of such failure (but in no event in excess of $1,000 per request).".
DRC's primary objective is to ensure plan's are timely responding to participants' and beneficiaries' requests for documents. This program assists in obtaining copies of a plan's Summary Plan Description and other documents as required. A plan administrator's failure or refusal to provide the requested documents, can result in penalty assessments of up to $1,000 per document request under ERISA Section 502(c)(6).
These cases are generally received by DRC as referrals from EBSA's Regional Offices, the Division of Technical Assistance and Inquiries (DTAI), or from plan participants and beneficiaries concerning the failure of plan administrators to provide requested plan information.
If the referral is from an EBSA office, there has generally already been a number of informal attempts to procure the documents prior to referral to DRC.
Blackout Notice – 502(c)(7) Program
In light of the events surrounding the Enron and WorldCom scandals and bankruptcies that resulted in many investors and plan participants losing a significant amount of there retirement savings, Congress enacted the Sarbanes Oxley Act of 2002 (SOA) to enhance corporate governance and disclosure. Section 306(b)(1) of SOA amended section 101 of ERISA adding new subsection (i) and section 306(b)(3) of SOA amended section 502(c) of ERISA by adding new paragraph (7).
The goal of the 502(c)(7) blackout notice enforcement program is to ensure that plan administrators are complying with the blackout notice requirements. These requirements were developed to ensure participants and beneficiaries are properly notified of restrictions to their accounts and afforded time to make informed decisions about their investments.
The blackout notice rules the disclosure requirements of ERISA by requiring plan administrators to notify participants in advance of when access to their plan accounts is being temporarily restricted, thereby affording participants ample time to evaluate and make informed decisions regarding their plan accounts before access to their account is restricted.
Section 101(i) of ERISA requires that plan administrators of individual account plans (except for one-participant retirement plans) provide notice to affected participants and beneficiaries in advance of the commencement of any blackout period. Section 502(c)(7) of ERISA establishes civil penalties for a plan administrator's failure or refusal to provide timely notice of a blackout to participants and beneficiaries. These blackout notice provisions of ERISA became effective on January 26, 2003 and are applicable to any blackout period commencing on or after that date.
Blackout Notice Requirements
In general, the term "blackout period" is a temporary suspension, limitation, or restriction (lasting more than three consecutive business days) of plan participants and beneficiaries ability to direct or diversify assets in their accounts, obtain loans from the plan, or obtain distributions from the plan (know as "affected rights"). Plan administrators are required to provide written notice to affected participants and beneficiaries at least 30 days, but not more than 60 days, in advance of the last day such participants and beneficiaries could exercise the affected rights, unless one of the exceptions provided apply.
The contents of the written notice must meet the requirements of Department Regulation section 2520.101-3(b)(1). As per the regulations, the notice shall contain the following:
- Reason(s) for the blackout period;
- Description of the specific rights affected;
- Length of the blackout period by reference to either,
- the beginning and ending dates of the blackout period, or
- the calendar week(s) during which the blackout period began and ended. (If calendar week(s) is/are referred to, the notice shall instruct affected P and Bs where during such weeks, they can easily and free of charge find out if and when the blackout period has begun or ended.);
- If investment rights are affected during the blackout period, the notice shall include a statement that Ps & Bs should evaluate the appropriateness of their current investment decisions;
- If less than 30 days advance notice was given, the notice must include a statement that Federal law generally requires 30 day advance notice and explanation why such notice could not be provided. (Exceptions to this requirement are noted below.);
- Name, address and phone number of the Plan Administrator or other relevant contact.
On occasions, this 30-day advanced notice does not apply. ERISA section 101(i)(2)(c) allows for two exceptions, noted below, provided a determination of the circumstances is made in writing, signed by a fiduciary of the plan, and the notice is provided as soon as reasonably practicable. The exceptions are:
- A deferral of the blackout period would violate the requirements of section 404(A) or (B) of ERISA. This exception allows for the fiduciaries of the plan to determine that it would neither prudent nor in the best interest of the plan and its participants to delay the start of the blackout for the purpose of providing the 30-day advance notice; or
- The inability to provide the 30-day advance notice is due to events that were unforeseen or circumstances beyond the reasonable control of the plan administrator.
A final exception is found in ERISA 101(i)(3) which states if the blackout period applied only to Ps & Bs in connection with their becoming, or ceasing to be, Ps or Bs of the plan due to a merger, acquisition, divesture or similar transaction of the plan or plan sponsor the notice must be provided as soon as reasonably practicable.
As per ERISA 101(i)(7)(B), a blackout period does not include a suspension or restriction which:
- occurs by reason of the application of the securities laws;
- is a change to the plan which provides for a regularly scheduled suspension disclosed to participants;
- applies to individuals pursuant to a qualified domestic relations order.
502(c)(7) Penalties
Pursuant to ERISA Section 502(c)(7), the Department has the authority to assess civil penalties of up to $100 a day for each separate violation against administrators of an plan who failed or refused to provide notice to participants and beneficiaries in accordance with ERISA Section 101(i).
The Department's regulations define "a failure or refusal to provide a notice" as a failure or refusal, in whole or in part, to provide notice of the blackout period to an affected plan participant or beneficiary at the time and in the manner prescribed by Section 101(i) of ERISA. Such a failure or refusal to provide a notice of blackout period with respect to any single participant or beneficiary shall be treated as a separate violation. Therefore the penalty is calculated for each affected participant or beneficiary (i.e. $100 per day per participant).
For purposes of calculating the penalty assessment, the date of failure or refusal occurs 30 days prior to the last day on which affected participants and beneficiaries could exercise the affected rights and continues through the end of the blackout period.
The Office of the Chief Accountant, with assistance from other members of EBSA, has administratively determined and developed a proposed schedule of penalties, within the 502(c)(7) framework, for blackout notice violations. A worksheet and proposed penalty structure have been developed to aid in penalty calculation.
